Latest Blogs
Baraka Hospital: Visiting a Nascent Surgical Program in the Massai Mara of Kenya

In 2015 the Lancet Commission on Global Surgery was convened with the goal of trying to achieve a comprehensive and thorough understanding of the challenges that impact the delivery of surgical care on a global scale as well as start to map a plan that addresses solutions. It is estimated that somewhere between four and five billion people may in fact lack adequate access to surgical care around the world. Death from this lack of access significantly outpaces the combined burden of malaria, TB and HIV annually.
While that may seem at first glance implausible, if one steps back and thinks of ‘surgery’ beyond the more simplistic notion of having a room with some equipment, someone available to perform the surgery and another to provide anaesthesia it starts to makes sense. My experience last year in Malawi working with Dignitas International supports this. To really be able to deliver complete surgical care includes addressing the issues of timeliness, expertise, safety and cost. A hospital needs to be able to evaluate acuity in the community, bring that patient in for assessment, have them medically optimized for the OR and then have a team ready to perform what is needed both safely and effectively. While absolutely essential to addressing many health challenges, surgery, when not properly considered or implemented can prove lethal. A summary of the Lancet Commision findings can be seen in this short video:

 It was with this in mind that I made a visit to Baraka Hospital in Narok County, which resides in the magnificent Maasai Mara region of Kenya. With 21 years of consultant surgical experience in practice and a reasonable understanding of the factors that drive surgical outcomes I travelled to learn, provide some teaching, reflect a little and then aim to learn some more
It was with this in mind that I made a visit to Baraka Hospital in Narok County, which resides in the magnificent Maasai Mara region of Kenya. With 21 years of consultant surgical experience in practice and a reasonable understanding of the factors that drive surgical outcomes I travelled to learn, provide some teaching, reflect a little and then aim to learn some more
Baraka Hospital is one of the indisputable jewels of the extraordinary We organization. With two decades of experience in the developing world it is a Canadian-based organization that works to try and improve the lives of communities around the world. Many Canadians are familiar with the passion and commitment of its founder, Craig Kielburger. The remarkable story of how he came to be an incredible driver of postive change around the world is worth exploring. We’s mission is rooted in the philosophy of enabling communities over time to become independently sustainable. By providing a ‘hand up’ and not a ‘hand out’ it relentlessly pursues a vision anchored on a belief that this can be achieved through five crucial pillars of community building. By focusing on education, heath, food, water and ultimately economic opportunity, entire communities can strive to be lifted from the hopelessness of oppressive poverty. A further understanding of this unique organization's philosophy and mandate can be found here:
Baraka Hospital, central in its location within this region of Kenya, has developed as an anchor that now provides healthcare to several of the communities that have been supported by We. From a simple clinic at the beginning to a hospital designation over the last few years, it has now reached the point where both an inpatient suite and two operating rooms have been developed. With the launch of surgery services set for next month, I went to Kenya hoping to evaluate what was being planned, provide some education to the staff and identify any obvious issues that may not have been addressed. I also wanted to see how Baraka was developing its surgery program in the context of the larger issues that plague surgery globally.
What I found was impressive. It was really exciting to be able to get some insight into a surgical program at its beginning. I met Michelle Hambly, the country director and many of the clinical staff that work in this hospital. It is through her leadership that a level of dedication, willingness, passion and commitment to good patient care exists across the facility. 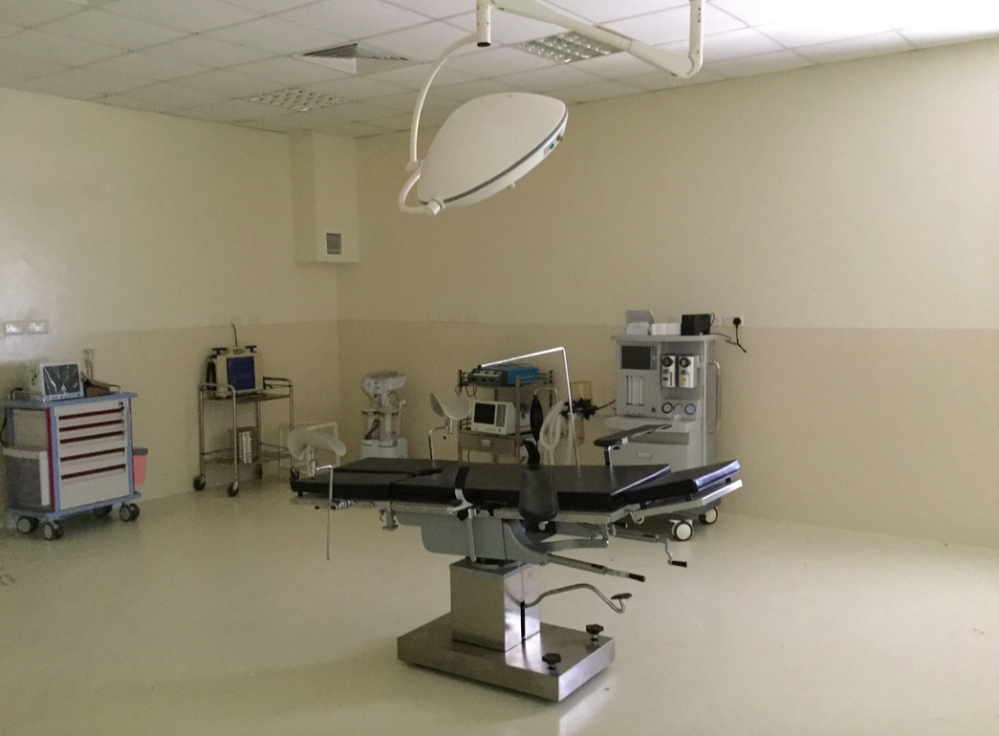 Correctly, the hospital has targeted only the bellwether surgical procedures that are recognized as essential in providing surgical care in low and middle income countries. If only C-Section, laparotomy and fracture surgery can be made available, millions of lives can be potentially saved around the world. Currently a mother labouring at Baraka who fails to progress must be taken down rocky road by ambulance to another facility an one hour away to undergo C-section. This can now be delivered on site and potentially earlier in labour, reducing both complications of childbirth and maternal mortality. Similarly, expertise in performing laparotomy to address common conditions such as appendicitis and fracture surgery to treat the large number of injuries secondary to motorcycle accidents will be performed. I found at Baraka a good understanding of the need for at least some form of a preoperative evaluation process. Finally the surgical and anaesthetic staff seemed adequate for what was being planned
Correctly, the hospital has targeted only the bellwether surgical procedures that are recognized as essential in providing surgical care in low and middle income countries. If only C-Section, laparotomy and fracture surgery can be made available, millions of lives can be potentially saved around the world. Currently a mother labouring at Baraka who fails to progress must be taken down rocky road by ambulance to another facility an one hour away to undergo C-section. This can now be delivered on site and potentially earlier in labour, reducing both complications of childbirth and maternal mortality. Similarly, expertise in performing laparotomy to address common conditions such as appendicitis and fracture surgery to treat the large number of injuries secondary to motorcycle accidents will be performed. I found at Baraka a good understanding of the need for at least some form of a preoperative evaluation process. Finally the surgical and anaesthetic staff seemed adequate for what was being planned
Perhaps what was most gratifying was witnessing what seemed to be an almost at insatiable desire to learn, embrace a culture of safety and respect in the operating room and an excitement to get the project started the right way. The most well-received talk I gave was on the surgery safety checklist and the need to empower all members of the team to speak up and if needed hold the start of a case if a problem is identified. With this in mind I think Baraka will be successful, allowing We an opportunity to hopefully scale it with time. It is very much in line with the principles that were outlined in the 2015 Lancet commission.

Community Outreach Team

With Michelle Hambly
I look forward to tracking its success as I continue to explore the massive surgical challenges that will continue to affect so much of this world. I will be in Uganda next week and will aim to write about a urology experience while there.
Rajiv
Comments
Posted: February 05, 2017
By: Errol Superville, MB
Three cheers to you again, Dr. Rajiv for making a difference not only in your practice of Urology with special interest in Ca of Prostate, at the Michael Garron Hospital in Toronto, but also to see you spread your knowledge and expertise in so many parts of the world, Mali, Nigeria, Uganda. Your keen interest forces me to ask myself the question, "am I doing enough to help my fellowman?" My wife, Patricia and I are on a cruise ship 'The Azamara Quest' at present sailing the Pacific Coast from Costa Rica to San Diego. Perhaps, I will make it my quest to do as much as I can to help others.
Thanks again, Rajiv.
From Errol.
Posted: February 06, 2017
By: Joy Gooding
Thank you for providing reports from your time in Africa. It is very gratifying to hear of the good work many are doing to see improve the health outcomes for people around the world. I wish the staff at Baraka and the communities they serve the best as they embark on this next step in their health care journey.
Posted: February 06, 2017
By: Lisa Lemon
Thanks for sharing Rajiv.
Posted: February 06, 2017
By: John
Well done Rajiv! A wonderful read and we are looking forward to learning about Uganda.
Posted: February 06, 2017
By: David Fraser
Looks and sounds amazing Dr. Singal.
Posted: February 06, 2017
By: Patricia Campbell
Rajiv,
Great job! I truly admire your unfailing dedication to be an ambassador advancing safe surgery through the use of the
"surgical safety checklist" You want others to be on board.
In spite of all the challenges, you constantly remind that we still can deliver the best professional care in such a time as now.
Posted: February 20, 2017
By: Doug Farley
Hi RS:
Thanks for well struck article.
I see that the average income in your area is under $2 daily.
So without outside charitable influence one can see that the medical goals will probably not happen.
As unlikely the central government has the money to do it.
Trust you're safe and secure?
Cheers and Ciao
Douglas G. Farley
Posted: February 20, 2017
By: Peter Jensen
Beautifully written Raj.....passionate and articulate.....how woefully inadequate so much of the world is in this regard.....the five pillars are essential and education is, in my opinion, at the fore.....education inevitably provides freedoms that support and enhance the other pillars.....and begets the insatiable quest for more education.
Bravo and I look forward to your next report....although I'm sensing it may be a bit gloomier.
Cheers
Peter
Posted: February 20, 2017
By: Joe Manget
Rajiv - as usual very inspiring. Thank you for sharing.
It's a very pragmatic approach - a focused set of surgical procedures that will make the biggest difference. That's why it will work. You aren't trying to solve everything at once. Congratulations.
Joe
Posted: February 25, 2017
By: Tom Moore
Rajiv
Amazed to learn the numbers and impact on the lack of surgery.
Your trip with WE sounds so successful and I imagine the first of
many.
Congratulations
Tom
Posted: March 26, 2017
By: Bob Eisenberg
The program reminds me of Save a Child¹s Heart. It's amazing how big the bang for the buck can be on an initiative like this one.


Posted: February 05, 2017
By: Fred Appleton
Aside for the obvious reason - I am honoured to have know you just a little bit. At the time when I and my family needed you, I was really was uncertain of the commitment of the health care system. You changed that. Thank you for doing what you do (and keeping me informed). All is well see you in the Spring.